Plantar fasciitis
What is it?
Plantar Fasciitis (pronounced plan-tar fash-ee-eye-tis) is a common cause of heel and foot pain in adults. Plantar Fasciitis means the bottom of the foot; Plantar Fasciitis is a type of connective tissue, and means inflammation.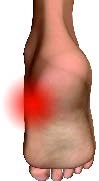
The classic symptoms of plantar fasciitis include heel pain that is usually most severe first thing in the morning. This condition is characterized by inflammation at the insertion point of the plantar fascia on the heel bone. Plantar fascia is a layer of tough fibrous tissue that runs along the bottom of your foot and supports your arch. This is one of the longest and strongest ligaments in the body. As the plantar fascia pulls on the heel, your body will respond by laying down more bone in the area. This can be seen on an x-ray and is known as a heel spur.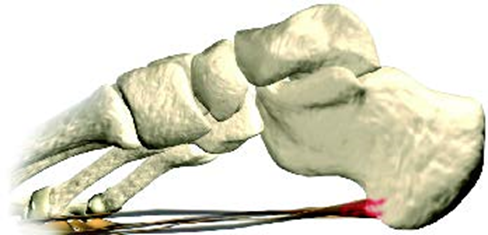
How did I get it?
Common contributors to this condition include: progressive flattening of the arches over time (primary reason); lack of flexibility in the calf muscles; changes in activity levels; overuse; and weight gain. When your arch drops, the plantar fascia begins to tear away from its insertion at your heel. When this happens over a long period of time, it can overcome the body’s ability to repair it-self.
How is it treated?
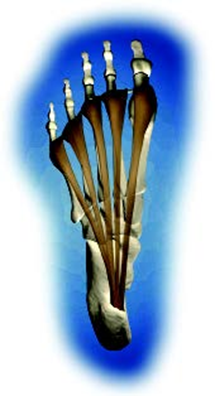
There are two main concepts in the treatment of plantar fasciitis: 1) the decrease of inflammation and 2) addressing the cause of the condition.
Stretching and Exercise: Stretching exercises are aimed at lengthening the plantar fascia in an attempt to lessen the pull on your heel. Increasing the length of the calf muscles is a very important part of any treatment. Tightness in this muscle group can cause excess pronation (arch drop), which may contribute to plantar fasciitis.
Anti-Inflammatory Agents: These may include ice and oral anti-inflammatory medications. These may provide some temporary relief from the pain of inflammation:
Night Splints: A device worn at night to prevent contraction of the plantar fascia and to maintain calf flexibility. These will usually lessen the “first step in the morning” pain and relieve symptoms temporarily. They can be uncomfortable to wear for some, but generally provide some relief.
Genuine spur
Corticosteroid Injections: This involves the injection of a steroid directly into the heel and site of inflammation. Usually reserved for intractable or difficult cases, this may provide more relief than oral medications. Talk to your doctor about the indications and risks for this treatment.
Extracorporeal Shock Wave Therapy: A high or low frequency sound wave is delivered to the area in an attempt to speed the healing process. Usually 1 to 3 treatments are required, and depending on the intensity of the sound wave an anesthetic may be used. The outcomes of this treatment are unproven and you should discuss the risks with your doctor.
Surgery: In cases that do not respond to conservative measures, surgical release of the plantar fascia may be a consideration. Cutting the plantar fascia will lessen the pull on the heel, but may have long term consequences including further flattening of the arch (since the plantar fascia con-tributes about 30% to the stability of the arch).
Foot Orthotics: The right custom orthotics are often the best defense in the prevention of plantar fasciits and the most reliable long-term cure for existing conditions. A Sole Supports orthotic, unlike typical custom orthotics, is designed to completely support the corrected arch of your foot, determined by a unique way of capturing your optimal foot position. A restored arch significantly reduces the daily pull on the plantar fascia by relaxing the ‘bowstring” function of the fascia. It is the only practical way to address both the symptoms AND the cause of your problem.
How long will it take to heal?
If left alone, plantar fasciitis can take from 6 to 18 months to heal. This can be frustrating, interfere with your ability to work and other activities, and the problem can come back. With Sole Supports custom, calibrated foot orthotics, you can expect either a dramatic loss of pain within the first weeks of use or a more gradual reduction of symptoms, depending on how long the problem has existed, normal body weight or how well you follow other therapeutic regimens prescribed by your provider.


